Doctors Should Talk To Patients About How They Want To Die, Says Regulator
James Meikle, The Guardian (May 20 2010)
The last month’s worth of news coverage in the UK has focused on nothing but the May elections so it was good to see an old fashioned death and dying story in the Guardian. My first take on these new guidelines, that doctors should speak with dying patients about, um, dying, was a smirk.
I do know, however, that frank and candid conversations about dying are not everyone’s forte, so I appreciate what the UK’s General Medical Council has done. As the Guardian reports,
While the guidance does not address assisted suicide, the GMC says it is still illegal and doctors have to remain within the law. However, it says there is “no absolute obligation to prolong life irrespective of the consequences for the patient, and irrespective of the patient’s views.”
This has been causing some real gnashing of teeth today. And it should. While it is absolutely true that the prolongation of life is never absolute, it’s still something which most doctors will do. Enter, then, patients and their end-of-life wishes. At a certain point during medical treatment, a patient may very well say “I’ve had enough and I want to stop all this.” Patients also expect (as well they should) that doctors will continue to treat them without giving up. The whole situation, then, can be a real bind for doctors and patients alike.
What these new guidelines want to do, it seems, is say to UK doctors that it’s ok when patients die, assuming the patient has a terminal condition and that the patient has accepted death. Negotiating the end of life is a complex task, especially when it comes to medical care, so I think that what the GMC has done is a good thing.
Here is a stripped down list of what the new guidelines entail:
• Doctors must give patients approaching the end of life the same quality of care as all other patients.
• Decisions must start from a presumption in favour of prolonging life.
• Doctors may recommend particular treatment options they believe best for patients, but must not pressurise them to accept advice.
• Patients who feel under pressure from families or carers to accept or refuse treatments must be helped to reach their own decisions.
• Doctors must not base treatment decisions involving significant risk to patients solely on constraints of money, staff or equipment.
• Doctors must respect “as far as possible” wishes of patients who do not want to know in detail about their condition or treatment.
• Doctors can withdraw from providing care if religious, moral or other personal beliefs amount to a conscientious objection to a patient’s decision to refuse treatment.
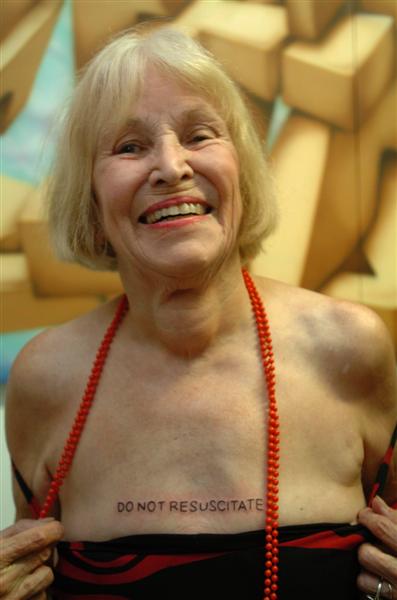 The new guidelines also reminded me, for some odd reason, of a funny and poignant story from late 2008. A 79 year old New Zealand woman, Paula Westoby, had Do Not Resuscitate tattooed on her chest. She did this so that in the event she unexpectedly died, her wishes would be known.
The new guidelines also reminded me, for some odd reason, of a funny and poignant story from late 2008. A 79 year old New Zealand woman, Paula Westoby, had Do Not Resuscitate tattooed on her chest. She did this so that in the event she unexpectedly died, her wishes would be known.
This is what I call a real commitment to the End of Life.